Rwanda | Overview
Improving the Health and Wellness of Vulnerable Youth in Rural Rwanda
Challenge
The Agahozo-Shalom Youth Village (ASYV) in Rwamagana, Rwanda was built in 2007 to provide a safe and secure environment for youth orphaned during the Rwandan genocide. As the village continues to grow, supporting about 500 youth per year, ASYV was looking to expand its health and wellness program.
Where We Started
The clinic is staffed with one full-time and one part-time nurse and four psychosocial workers. The clinic needed protocols to guide their daily activities for first aid and preventative care. This included adding mental health and first aid skills for the village staff.
Our Impact
Collaborating with the Health and Wellness team, we worked together to standardize and expand the annual physical health assessment to include nutrition and mental health screening, which is now done annually for each student. An algorithm to evaluate and treat children who have fever was created and used an example to develop further algorithms to manage common pediatric ailments. First aid training was taught to all staff. Local Course Trainers received additional education regarding how to facilitate the course and training materials were provided to the Trainers to be used in their first aid courses for staff. In addition, first aid kits were donated and distributed to common areas and homes around the village.
Moving Forward
Since our time in Rwanda, we continue to be available to share our expertise as issues arise. We also serve as board members on the Health and Wellness Committee and meet quarterly to discuss ongoing issues and developments in the village.
Contact
Kathryn Barrandon, Global Nursing Fellow; Michele Morin, Global Nursing Fellow
Improving Pediatric Hospital Triage
Challenge
Kirehe District Hospital is a public hospital in rural Rwanda, with a busy general pediatric ward with severe understaffing — around 30 pediatric patients are often covered by only two nurses.
Where We Started
Through the Boston Children’s Global Health Delivery Fellowship, Shela Sridhar, MD, worked with pediatric nurses and hospital leadership to implement a Pediatric Early Warning Score in Rwanda, a tool that uses vital signs and a physical exam to recognize children who are at risk of becoming very ill. Early warning scores are not widely utilized in resource limited settings. With the assistance of Boston Children’s nurses, a curriculum was developed and implemented to assist local nurses and physicians to identify critically ill children for early intervention.
Our Impact
Through our curriculum we were able to see an increase in the number of early transfers to higher level of care keep kids safe and preventing life threatening events. It also improved nursing feelings of empowerment in their skills and ability to communicate their findings to physicians.
Moving Forward
Through the Global Health Delivery Fellowship, subsequent pediatric fellows will be able to build on the initial foundation of training to quickly recognize children who are becoming sicker or having life threatening complications. Fellows will continue to work on training physicians and pediatric nurses on more complex medical decision making in triage and management for patients who need more intervention.
Contact
Shela Sridhar, Global Pediatrics Service Delivery Fellow
Electricity-free Infant Baby Warmer
Hypothermia, or low body temperature, in infants remains a leading cause of neonatal mortality even in places with warm climates such as sub-Saharan Africa and South Asia; underweight and premature babies are particularly susceptible to hypothermia. Dr. Anne Hansen, MD, MPH, the medical director for Boston Children’s Hospital’s Neonatal Intensive Care Unit, has been working with collaborators at Lawrence Berkeley National Laboratory’s Institute for Globally Transformative Technology (LIGTT) to develop a warming pad that can keep a newborn warm for hours at a time without the need for electricity making it ideal for a resource-limited setting. To warm the pad, Hansen has turned to something all cultures can access: hot water. The warming pad is made up of a “phase-change” material that can retain heat for hours. Its plastic coating can easily be washed with soapy water, making it readily reusable. A prototype of the pad has already been developed and shown to health care providers in Rwanda, where Hansen is working to study its safety and efficacy. Although it’s not ready for mass production, Hansen hopes to design the infant warmer so it could be manufactured locally, allowing Rwandans to produce and sell the pads on their own terms. And if she can keep the price point low enough, hospitals, clinics, and midwives could potentially purchase multiple pads, warming one up as another cools and keeping a newborn warm for days on end. As Hansen says, “Babies should not be dying of hypothermia. This has to be a fixable problem.”
Improving Surgery Systems in Rwanda
A major barrier to improving surgical access and outcomes is the lack of research capacity in Low to Middle Income Countries (LMICS). Recognizing this, Dr. Yihan Lin from the Program in Global Surgery and Social Change (PGSSC) has worked in Rwanda to help develop a complete curriculum for operational research training (ORT). ORT is a rigorous research training method, which develops research on key operational issues while simultaneously building local research capacity. This course is spaced over three modules within the course of eight months to allow time to complete critical milestones in between each module. The three modules will consist of:
- protocol development
- data cleaning/analysis
- manuscript preparation.
Research fellows serve as facilitators for ORT, providing mentorship in all phases of the ORT.
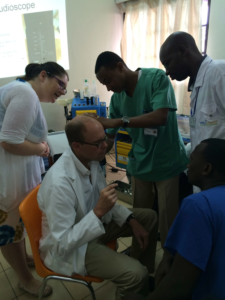
Teaching Otolaryngology in Rwanda
Rwanda is underserved from an ORL perspective, with just 4 faculty in the whole country who are equipped to train the residents who will serve a population of over 11 million. Dr. Roger Nuss and Dr. Julie Strychowsky are creating a template of teaching and training in ORL for resource-poor settings through Oto-Simulation (an ear examination simulator), teaching cases, and through teaching diagnostic tools. This initial partnership with University Teaching Hospital of Kigali (CHUK) in Kigali, Rwanda serves as a template that can be duplicated in resource-poor settings to increase accessibility to ORL teaching skills.
