Gynecomastia | Symptoms & Causes
What are the symptoms of gynecomastia?
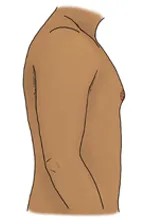
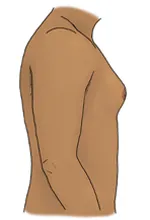
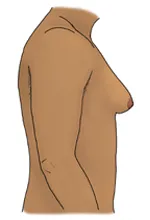
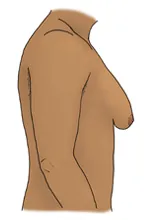
The most common symptoms of gynecomastia are enlarged breast mounds that can be painful or tender. The breast mounds may also feel rubbery or firm.
What causes gynecomastia?
Gynecomastia is most often caused by hormonal changes during puberty, but it can also be a result of or exacerbated by genetics, obesity, or certain medications and drugs.
In rare cases, gynecomastia can be caused by a tumor or certain genetic disorders and conditions, such as Klinefelter syndrome, a condition in which male babies are born with an extra X chromosome.
Gynecomastia | Diagnosis & Treatments
How is gynecomastia diagnosed?
To rule out any underlying disorders or conditions, your child’s physician will ask about their health and medical history and do a physical exam.
How is gynecomastia treated?
In most cases, no treatment is needed for gynecomastia because the breast gland diminishes during puberty. However, if gynecomastia continues for more than two years without any improvement, we will work closely with Adolescent and Young Adult Medicine and Endocrinology to explore other causes, such as hormonal imbalances.
Non-surgical care for gynecomastia
Non-surgical care for gynecomastia includes emotional support, compression shirts and, in some cases, medication.
Surgical treatment for gynecomastia
We consider surgery for gynecomastia when no further involution is expected based on your child’s age and development, or when excessively large or abnormal breast growth causes pain or interferes with your child’s quality of life.
Surgical techniques include:
- Liposuction
- Surgical tissue removal
- Peri-areolar incision: Glandular and fatty tissue is directly removed through an incision along the lower perimeter of the areola.
- Double incision and free nipple grafting: After an incision is made, excess glandular, fatty tissue, and skin is removed to achieve a male-appearing chest contour. Nipple grafting involves removing the nipple and placing it back on to the chest as a skin graft.
- Other techniques: Your child’s surgeon will discuss whether other surgical options are the best fit.
What to expect after surgery
Full recovery from gynecomastia surgery typically takes four to six weeks. Most patients return to school and light activity about a week after surgery. Your child’s care team will work closely with you and your child to navigate the best recovery plan.
During the first week after surgery, your child will need to wear a snug compression vest continuously. Bathing or showering must be modified to keep the vest dry all the time. In some cases, drainage tubes are placed during the surgery and may need to stay in place for one week. Drains are removed in the surgeon’s office.
Plan on limiting physical activity such as exercising, weightlifting, and other sports for four to six weeks after surgery. Your child’s surgical team will discuss specific restrictions based on your child’s activities.
How we care for gynecomastia
The Adolescent Breast Center at Boston Children’s Hospital is one of the first in the country dedicated exclusively to evaluating and treating breast disorders and conditions in children, teens, and young adults through surgical and non-surgical treatments. Our program includes providers from surgery and plastic surgery, adolescent and young adult medicine, and social work who work together to treat all physical and psychological aspects of gynecomastia.