Idiopathic Scoliosis | Symptoms & Causes
What are the symptoms of idiopathic scoliosis in kids and teens?
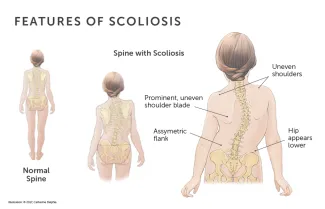
During a child’s growth spurt, the signs of idiopathic scoliosis often become more noticeable. These include:
- uneven shoulders
- one shoulder blade protruding more than the other
- ribs more prominent on one side
- uneven waistline
- difference in hip height
Idiopathic scoliosis is often first discovered during a pediatric checkup or school screening. This is particularly true in children who wear loose-fitting clothes that might cover up the symptoms. If a pediatrician or school nurse suspects your child has scoliosis, they may recommend an evaluation by a pediatric orthopedist or spinal specialist.
What causes idiopathic scoliosis in kids and teens?
There is no definite cause of idiopathic scoliosis or way to prevent the spine’s tendency to develop a side-to-side curve. Idiopathic scoliosis may run in families, but researchers have not confirmed this.
Idiopathic Scoliosis | Diagnosis & Treatments
How is idiopathic scoliosis diagnosed in kids and teens?
Clinicians who suspect idiopathic scoliosis conduct a detailed medical history and physical exam to confirm the diagnosis. During the physical exam, the doctor may use the Adam's forward bend test to detect abnormal curvature of the spine. For this test, your child bends forward from the waist, hangs their arms loosely in front of them, and reaches for the floor. If your child has scoliosis, one side of their rib cage will be more prominent than the other. The doctor may also order an x-ray, which allows them to see an image of the spine.
What are the treatment options for idiopathic scoliosis?
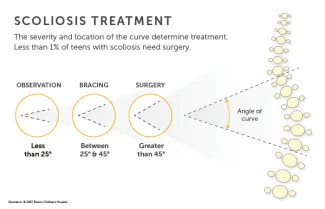
Treatment for idiopathic scoliosis depends on a number of factors, including your child’s age, severity of their spinal curve, location of the curve, and the pattern and progression of the curve. In many instances, simple observation is the first form of treatment.
Children with mild scoliosis, a curve of less than 25 degrees, are typically monitored at regular doctor visits to be sure the curve does not get worse.
Children with moderate scoliosis, a curve between 25 to 45 degrees, are typically treated with bracing. The brace keeps the spine in a straighter position as the child grows. This can either partially correct the curve or prevent it from becoming more severe. If the curve gets worse despite bracing, the child will probably need surgery.
Children with severe scoliosis, a curve greater than 45 degrees, usually need surgery. The most common surgical procedure is a spinal fusion. For this procedure, the surgeon uses metal rods, hooks, screws, and wires to correct the spinal curve and secure the spine in a straight position while the fusion heals and becomes solid.
What is the long-term outlook for kids and teens with idiopathic scoliosis?
Idiopathic scoliosis is not a life-threatening condition. Most children and adolescents with idiopathic scoliosis can look forward to normal, active lives. Your child’s outlook depends in large part on the nature and severity of their scoliosis as well as their age. Early diagnosis and treatment are important components of minimizing the long-term effects of scoliosis.
How we care for kids and teens with idiopathic scoliosis
The Spine Division at Boston Children’s Hospital is the largest and busiest pediatric spine center in the United States. Our spine specialists see thousands of spine patients and perform hundreds of spine surgeries each year. We treat all types of scoliosis and other spine conditions, from the most common to the most complex.
With early intervention, the majority of our patients are treated successfully with bracing and other non-invasive treatments, including physical therapy and Schroth therapy. The most widely used brace for scoliosis, the Boston Brace, was developed at Boston Children’s more than 40 years ago. While we are proud of this legacy, we work closely with our patients and their families to determine which brace is right for them.
For children who need surgery, our surgical team includes surgeons, anesthesiologists, and nurses with specific skills and expertise in spine surgery. Each member of the team plays a role in ensuring quality and safety before, during, and after surgery.
Idiopathic Scoliosis | Patient Resources
Patient and family guide to scoliosis
This e-book for patients and families shares information about the diagnosis and management of scoliosis, and offers advice about how to live with the condition.
How to put on a Boston brace (video)
Dr. Timothy Hresko, from Boston Children’s Hospital Orthopedic Center, demonstrates how to help a patient with scoliosis put on a Boston Brace.
Embrace the brace digital slideshow
Patients and providers offer advice to help others with scoliosis thrive while wearing a brace.
How to support your child who has to wear a brace
Experts at Boston Children’s answer questions about what it’s like to wear a brace and how a parent can support their child when they have to wear one.


