Congenital Scoliosis | Symptoms & Causes
What are the symptoms of congenital scoliosis in toddlers and children?
Although congenital scoliosis is present at birth, it may not be obvious that a child has it right away. Congenital scoliosis often gets worse as a child grows.
Common signs and symptoms of congenital scoliosis include one or more of the following:
- uneven hip heights or positions
- uneven shoulder blade heights or arm lengths
- head not centered with the rest of the body
- left and right sides of the back appear uneven when the child bends forward
Children with congenital scoliosis may also have signs of other, related conditions, such as:
- hairy patch or dimples on their back
- rib hump or small bump on their back
- pain or spasticity in the lower extremities
- stiff neck or short neck or spine
- abnormally formed hand, arm, or foot
- difficulty hearing
- bladder or kidney problems
- other problems with the bones, muscles, or joints
What causes congenital scoliosis in babies?
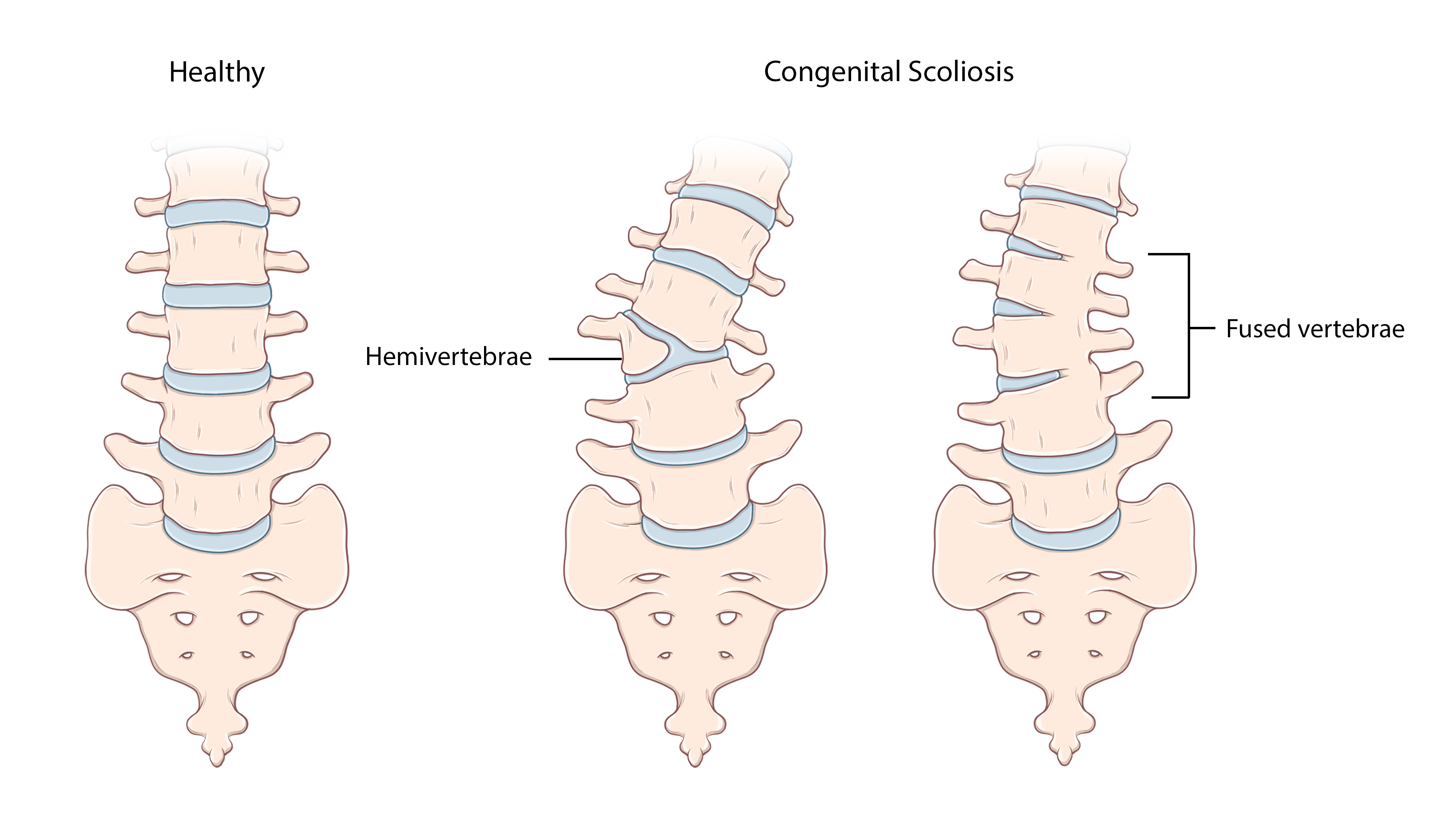
Congenital scoliosis occurs early in pregnancy, when one or more of the vertebrae in the spine don’t form completely. This can cause a sharp angle — called a hemivertebrae — to develop in the spine. In other babies, the developing spine does not fully separate into distinct vertebrae. As a result, two or more of the vertebrae may be partially fused. For some children with congenital scoliosis, spinal deformity is caused by a combination of these problems.
Congenital Scoliosis | Diagnosis & Treatments
How is congenital scoliosis diagnosed in toddlers and babies?
To diagnose congenital scoliosis, your child’s doctor will do a physical exam and take a complete medical history. The doctor may also order an x-ray in order to look more closely at the affected part of the spine.
Up to 30 percent of patients with congenital scoliosis have issues with their spinal cord as well. Your child’s doctor may order a magnetic resonance imaging (MRI) of the spine if they see any signs or symptoms related to spinal cord problems or if your child needs surgery.
Because congenital scoliosis is the result of abnormal development of the spine at eight to 12 weeks of gestation, your child’s doctor may order an ultrasound or echocardiogram to determine if other systems that develop at the same time were affected. These could include the urinary, genital, or cardiac systems.
What are the treatment options for toddlers and children with congenital scoliosis?
Your child’s treatment options will depend on their age, size, and the severity of their spinal curvature. Some children with smaller curves are monitored to see if their spine becomes more curved as they grow. If the curve remains small over time, the child may not need any further treatment.
When congenital scoliosis is severe enough to require treatment, the child usually needs surgery. Bracing and other types of non-surgical treatments are generally not effective for congenital scoliosis. The type of surgical treatment will depend on your child’s age and stage of growth.
Surgical options for toddlers and children with congenital scoliosis
Surgical options for young children with congenital scoliosis aim to keep the spine aligned and allow the child to continue growing.
- Growing rods are temporary implants that control spinal curvature as a child grows. The rods are attached to the spine with screws. About every six months, a surgeon lengthens the rods through a small incision in the back to allow the child’s spine to continue growing.
- MAGEC (MAGnetic Expansion Control) System is an adjustable growing rod system that uses magnetic technology to lengthen the rods without repeat surgeries. After an initial surgery to implant the MAGEC system, the surgeon periodically lengthens the rods using a remote control.
- Expansion thoracostomy/VEPTR™ is an expandable titanium rib used for children with underdeveloped chests. By keeping the chest wall expanded, the VEPTR creates room for the lungs to develop and the spine to grow straight.
Surgical options for tweens and teens with congenital scoliosis
Spinal fusion surgery is the most common surgical treatment for severe scoliosis in adolescents. The procedure straightens the spine and solidifies the bone so it will no longer curve abnormally. For six to 12 months after surgery, the spine fuses in much the same way that a broken bone heals. Your child may need to wear a brace during this time.
What is the long-term outlook for children with congenital scoliosis?
The outlook for congenital scoliosis depends on the nature and severity of the curve and other related conditions. For children with severe curves, successful spine surgery and attentive post-operative care will help their spines grow as normally as possible.
How we care for congenital scoliosis
The Spine Division at Boston Children’s Hospital is the largest and busiest pediatric spine center in the United States. Our spine specialists see thousands of spine patients and perform hundreds of spine surgeries each year. We treat all types of scoliosis and other spinal conditions, from the most common to the most complex.
Our surgical team includes surgeons, anesthesiologists, and nurses with specific skills and expertise in spine surgery. Each member of the team plays a role in ensuring quality and safety before, during, and after surgery.

